Last weekend, I had planned and prepared to swim to Rottnest solo for the first time. I had done the training, had my team prepped, and organised the logistics. Until the weather didn’t cooperate...
Athletes are no strangers to the physical demands of their chosen sports, but what many may not fully appreciate is the profound impact that stress can have on their performance and the potential to contribute to injury. We need to understand that stress is not merely a mental burden; it can manifest physically and significantly affect an athlete's overall well-being and athletic capabilities.
In a nutshell, food is required for your body to fuel exercise and a range of issues can result if intake is insufficient. Theoretically this seems like common sense, but in the performance driven sporting world ensuring adequate intake is not so simple. Do you find you get injured frequently? Are you often sick or experience other health issues? Do you have difficulty recovering from training sessions or achieving the results you should? If any of this sounds familiar a thorough review of your nutrition may be indicated.
Type 2 Diabetes (T2D) is typified by excessive glucose in the bloodstream, otherwise known as hyperglycemia (Sampath Kumar et al., 2019). This is linked to impaired metabolism of proteins, fats, and carbohydrates along with either insufficient insulin secretion or lowered sensitivity to the metabolic effects of insulin.
Achilles Tendinopathy (previously known as Achilles Tendonitis) is a condition commonly treated by Sports Physiotherapists. It frequently affects athletes from running and jumping based sports but may also result from every day life. The main complaint is of pain and/or stiffness localized to the mid-portion of the achilles tendon or at its attachment into the heel bone (calcaneum).
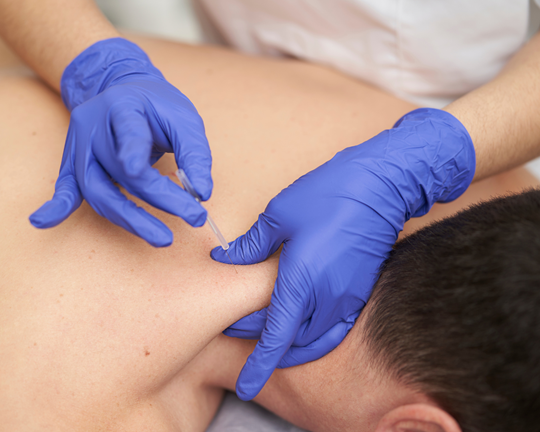
Dry needling is a therapeutic technique used by physical therapists to treat muscle pain, tension, and dysfunction by inserting thin, filiform needles into myofascial trigger points ("knots"). It aims to deactivate these spots, improving blood flow and flexibility.
Remedial Massage has been gaining recognition for its significant impact on health and wellness. This specialised therapy blends techniques designed to relieve pain, improve muscle function, and enhance overall well-being. With its wide range of benefits, you might be wondering how remedial massage can specifically help you?
Discover specialised physiotherapy services tailored for Australian football athletes at our Perth clinic. From amateur enthusiasts to professional players, our team is dedicated to addressing the unique physical challenges and injury risks associated with AFL.
As the pre-season excitement builds up for East Perth FC, Jordan Wilson at WA SportsMed Physio is diligently working behind the scenes to ensure the players are in prime condition for the upcoming season. Over the past month, senior players have been undergoing their annual pre-season screenings, a crucial step in optimizing performance and minimizing injury risks.
Welcome to Inside Combat Sports, where we dive deep into the world of combat sports such as Boxing, Muay Thai, Wrestling and Brazilian Jiu-Jitsu (BJJ). Whether you're an athlete, coach, or enthusiast, understanding the biomechanics, injuries, and training protocols is crucial for longevity and success in these demanding disciplines.
Pilates has gained immense popularity in recent years, and for good reason. Its unique blend of strengthening, flexibility, and mind-body connection offers many benefits for people of all ages and fitness levels. But with various types of Pilates classes available, how do you know which one is right for you?
Diastasis recti (also known as Rectus Abdominis Diastasis- RAD) is the separation of the abdominal muscles. It is a common issue, especially among women during and after pregnancy. As a physiotherapist specializing in women's health, addressing RAD requires a tailored and progressive approach.
Pregnancy is a transformative journey that brings about various physical changes in a woman's body. As a physiotherapist, the focus of pre and postnatal care is ensuring the well-being of both the mother and the developing foetus. The integration of physiotherapy into prenatal and postnatal care plans has proven to be beneficial in managing the physical challenges associated with pregnancy and facilitating a smoother recovery postpartum.
Have you rolled your ankle or injured your foot and had to spend time in a boot to allow the injury to heal ? Camwalkers (Moonboots) are used more and more commonly with ankle and foot injuries to protect the injury in their initial stages. During this time the pain for the athlete will reduce a lot, there may be things your physio or doctor allow you to do while in the boot. For example come out of the boot during the day to move the foot through all its movements, or perform calf work in safe positions.
Stretching, or the forceful lengthening or a muscle in order to reduce its tightness, has been around for thousands of years and is hardwired into the makeup of humans and animals alike. The first thing most people do in the morning (after pressing snooze on the alarm 5 times) is to let out a great yawn and stretch out all the muscles that have been dormant while you sleep. It is so instinctual that even the family dog and cat will do it!
The hamstring muscles consist of 4 muscles, with the long head of biceps femoris being the most commonly injured because of its long lever arm, involvement in multiple joint kinematics and muscle architecture. Each AFL club can expect an average of 6 hamstring strains per season, with a recurrence rate of around 13.5% per strain. This recurrence rate has been as high as 40% at the elite level in the last 20 years. (Orchard et al., 2013).
Need help with running related knee injuries or want to drop some time off of your PB?
With the the footy season around the corner, Fremantle Docker’s AFLW physio Gabby discusses the most common football injuries and gender differences between male and female footballers in a three-week blog series.
Part two of our blog series explores common injuries in AFL. As men’s football has developed into the fast, powerful game of today, the nature of injuries particularly soft tissue pathology, has changed. Interestingly the incidence of hamstring, hip and groin injuries have remained high for many years, highlighting the importance of injury prevention programs across all levels of football.
Come see a sports physiotherapist and there will inevitably be a discussion around strength work. Strength work is proven to benefit every body system, prevent injury and improve performance. Anyone who begins strength work should see an immediate increase in neuromuscular pathways and muscle activations patterns. But what happens after the immediate neuromuscular improvements plateau? If you are in the gym multiple times per week for most of the year how do you optimise each session to ensure you are getting the most out of your time? Marina has come up with some tips to maximise strength performance through your gym program.
Tom Valentine - Physiotherapist. Have you started a fitness or health goal for 2020? Good work! This can be trying to get more steps or general exercise into your day, or trying out a new sport or type of exercise.